Safe Buildings
Facilities Operations Platform
Leads: Samuel Fernandes, Raja Sengupta
Most American enterprises do not manage infectious diseases. Covid-19 is changing that. Enterprises are now asking for symptoms, conducting temperature checks, creating distancing and PPE use policies. Some, like universities and meat-packing plants even have their own SARS Cov-2 testing programs. The new business processes need to make clients and employees feel safe, shield enterprises from liability, but also achieve biologically real outcomes.
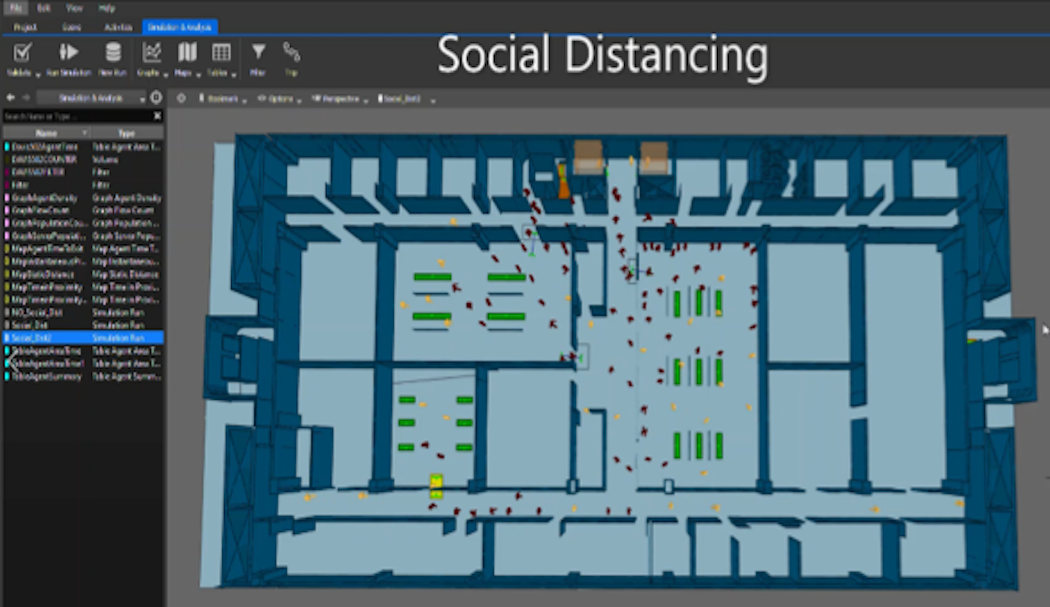
The ‘Covid-19 Facility Operations Platform’ aims to empower enterprises to measure exposures in enterprise facilities, reduce them and minimize the likelihood of disease outbreaks. We propose IoT data-driven analytical processes. We start with only three causal factors – PPE use, in-facility social distancing and air flows. Of the three modes of SARS Cov-2 transmission, i.e., contact-droplet, airborne-aerosol, and fomite; social distancing, PPE use, and air-flow strongly determine the first two, and thereby the risks of exposure borne by clients and employees on enterprise premises. Moreover, enterprises can manage their HVAC and who goes where within their facilities. The platform empowers enterprises to do the best they can on three management processes that matter and are also their responsibility.
Designing tools to monitor and mitigate exposures in enterprise facilities and minimize the likelihood of disease outbreaks

Metro Bots
Leads:
Sanjoy Chatterjee, Rakhi Basu
Ideation Technology working with World Bank group is using various forms of transportation data to optimize, predict and calculate the real-time arrivals and departures of public transport systems. We have leveraged this to develop a uniquely designed bot that can accomodate dynamic capacities on public transportation modes in a metropolitan region.
Currently, the team is deploying the bot technology on the Kolkata Metro system in India to keep the passenger count on trains under 400 per rake every trip to maintain social distancing norms. The boarding pass on the mobile phone of passengers will change its color every hour. This color code can easily be spotted by cops at transit statio entrance so they can allow passengers into the station as per the right time slot alloted. We see this as a first step towards seamless integration of all public transport modes.
Enable transportation with minimal risk to travellers and accomodating dynamic capacities using digital bots
Soteria4good
Leads:
Mark Bamford, Sarah Lewis
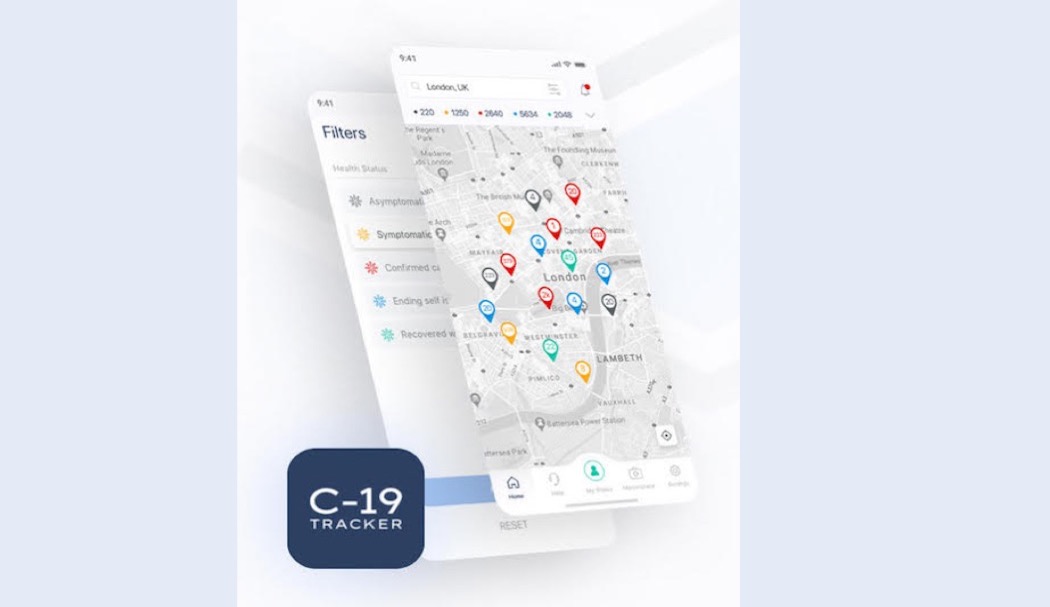
WHY? Our mission is to provide a tech platform that protects individuals, communities & businesses, allowing them to get back to generating social & economic value safely.
WHAT? The Soteria Platform that enables people to participate in the things they love & value, knowing that the environment they are in is as safe as possible. Allowing businesses to open & function so that people find a new normal faster.
HOW? An independent SaaS platform that enables businesses to regain their target audience’s trust by validating their COVID health status. We do this by privately and safely monitoring a person’s health status through self-diagnosis and verified testing prior to the desired activity.
Using technology to scale social and economic activity safely and rapidly using active health monitoring.

Understanding The Community
Team:
Hassan Obeid, Mohamed Bouzaghrane, Dan Chatman, Karen Frick, Raja Sengupta, Joan Walker, Daniel Rodriguez
Recent studies of household responses to COVID-19 have failed to collect data on the underlying structural and economic factors that condition people’s ability to comply with social-distancing and shelter-in-place rules. Such data are needed to mitigate the effects of the pandemic and to safely begin to open the economy. Through a research partnership with Embee Mobile, an industry leader in providing mobile insight solutions, we use a unique sample of more than 100,000 US mobile phone users, taking pre- and post-COVID movement data from GPS traces to measure changes in household activity patterns and correlate those with baseline demographics such as household income, household size, and race/ethnicity. We will then, over a minimum three-month period, repeatedly survey a subsample of individuals in ten metropolitan areas to measure economic well-being, mental health, personality, political orientation, and barriers to sheltering along with documenting changes in activity patterns from GPS traces. This novel research will enable future work on experimental interventions delivered via smartphones to improve compliance.
The research seeks to determine how households' ability and willingness to engage in risk-reducing behavior vary according to economic, demographic, occupational, and ideological factors. In the short term, understanding this will enable improved policy and targeted interventions to address health disparities surrounding COVID-19 social distancing in such a way as to also enable a safe opening of the economy. In the longer term, the information will be useful in informing behavior change programs aimed at preventing and managing infectious and chronic diseases.
Using a nationwide smartphone panel to understand population behavior and heterogeneity and inform intervention methods

Digital Contact Tracing
Lifeband - Contact Tracing Wearable Wristband
Lead: Anna Luisa Schaffgotsch
Contact tracing is exclusive to people who have access to mobile devices. With most people owning smart devices this seems to be an easily pervasive technology. Yet it causes an even bigger discrepancy between the digitally literate and digitally illiterate. Vulnerable members of the communities cannot participate in current safety methods provided to communities. However, they are the members of our community most at risk of coronavirus: elderly, disabled, children and families from low economic backgrounds. The Lifeband team wanted to offer a solution for these people to participate in contact tracing and offer digital equality to these members. The wristband is a low tech device that requires limited set up, does not have a screen, does not require charging and is affordable. Furthermore it captures data with military grade data security and offers location information vital to safeguarding our communities and building virus safe infrastructure. The aim of the devices is to restart inclusive living during pandemics. In this presentation we would like to present information about our works so far, the technical approaches taken and why they are vital for a safe solution and the outcomes we would like to achieve with our solution
Context Rich Approach
Leads: John Swartzberg, Raja Sengupta
Contact tracing involves interviewing the infected and persuading the person to adopt behaviors in the public interest, e.g. quarantine. The interview also aims to identify the people exposed to the infected person. The tracer then contacts the exposed and persuades them to adopt another behavior, e.g., go get tested. Therefore Digital Contact Tracing needs to be Persuasive or Behavior Change technology [Fogg 2002, Consolvo 2009], i.e., technology designed to the science of persuasion. The behavior of focus here is that of contact. This behavior, for each person, is their time history of contacts. The duration relevant to Covid-19 is the infectious period, nominally 14 days. Then for covid-19, the measurement period is 14 days. This measurement is our first technology development activity. Once we have the contact record, it will have many uses. The contact record becomes the record of exposures sought by public health should the person become infected. It embodies the costs of behavior change and becomes the means to derive the incentives, messages, or services that will induce quarantine or isolation behavior.
Some technologists view the contact record as a series of anonymous Bluetooth proximity identifiers, devoid of human or behavioral meaning. But a record devoid of context about its person will not support persuasion or behavior change. Instead our system builds a context rich contact record. Much like the travel diaries used in transportation to derive the value of providing new bus services or bike lanes, we seek to know what places the person has been and the activities therein e.g., work leisure, meet friends, exercise, and so on. Some of these visits entail personal interactions relevant to Covid-19 and others impersonal ones, e.g., the stranger adjacent in a coffee shop, or the bus passenger in the next seat. The people one lives with, or those in relations of intimacy, exercise buddies, dinner guest are the personal interactions and their details are sought in contact interviews to determine exposure and obtain contact information. The impersonal ones could be revealed by the kind of API being proposed by Apple and Google but the context surrounding the impersonal ones is also important and has public health value.
We seek to make the contact record just as rich as the one currently derived in contact interviews, as opposed to the faceless, anonymous contact record. Technology needs to produce the same context used by public health for infectious disease management. This kind of record is also the one that will enable an enterprise like our university to understand its avenues of contact and disease transmission in an actionable manner. Building the rich contact record involves two challenges. The first is a loss of privacy, something most of us fear, and the second the human or enterprise effort needed to build the record. Our solution addresses the privacy problem by keeping the record, by default, in the custody of its builder, the person whose behavior it records. The record can only be released by the person, its custodian. I may release my record to my public health department because I fear exposure. My public health department then becomes able to check my record against its own database of infections and advise me. I may also release my record to my public health department because I have become infected and seek to have the public health department inform the exposed without engaging me, or seek quarantine support from the department.
Developing technology to build context rich exposure record while addressing privacy challenges
Pandemic Surveillance
Data Driven Health
Leads: Sanjay Pudupakkam, Jack Rush
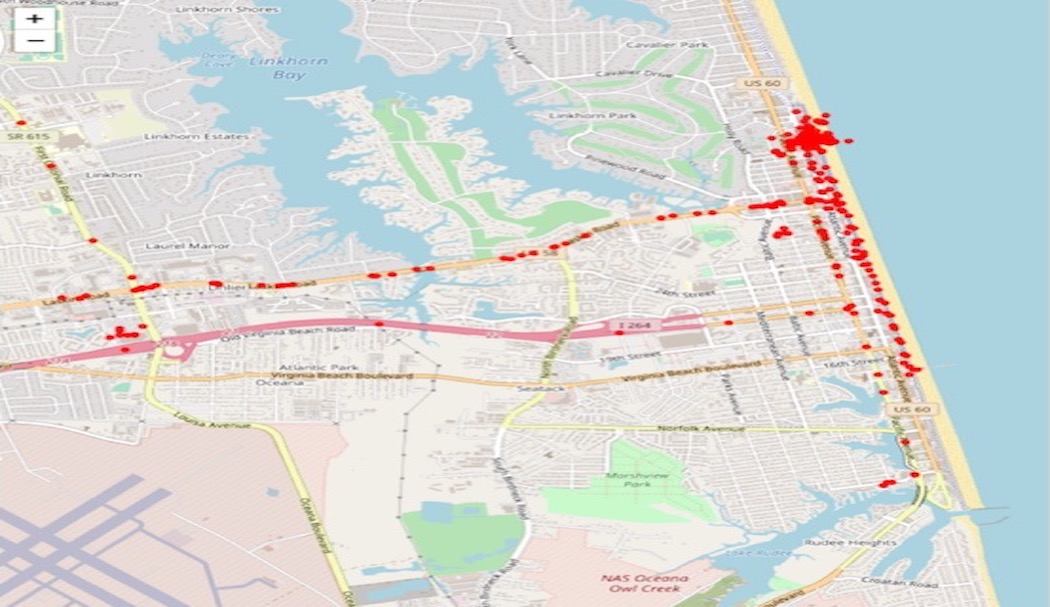
Data Driven Health is an AI Technology company that is transforming population health and syndromic surveillance. Its FluDemic™ AI Prediction Center is a free, interactive web-based solution that tracks influenza and COVID-19. FluDemic™ predicts potential outbreaks by utilizing proprietary artificial intelligence, giving the public a better understanding of what is happening in their community. The FluDemic™ AI Prediction Center sources a wide array of data feeds into proprietary machine learning algorithms that target and predict geographies that are the most susceptible for future surges, outbreaks, and socioeconomic risk for spread.
Safe Campus App
Lead: Christian Manasseh
Mobius Logic — a leader in next-generation digital services and consulting - helps organizations realize results in a digital world through business technology solutions and cloud-based services that combine insight, innovation, and expertise focused on the latest technologies. Leveraging the collective knowledge of SPM, Mobius Logic built the Safe Campus App that is used in the Safe Campus study to assess the effect of mobility in the spread of COVID-19. The Safe Campus study evaluates the risk of COVID-19 and community mitigation strategies to prevent COVID-19 transmission among students, workers, and essential workers at UC Berkeley. The Safe Campus app brings a new method of collecting data for public health consumption by engaging the user in a weekly raffle. This results in better quality mobility traces that help public health researches track the places visited by their study participants.
Mobius Logic is also pioneering an app that will assist users in moving around safely during a pandemic. Distance Factor is an App powered by AI to monitor and improve social distancing practices allowing communities to move around while being cognizant of their personal safety and the safety of others in their community. By calculating a Distance Factor Number for each person and place of business, Distance Factor empowers people to make decisions that keep them and their loved ones safe from transmitting and contracting COVID-19. For more information, please visit www.mobiuslogic.com
Estimate infections in real-time using existing and novel data streams in concert with data science-theoretic methods



































